Biomedical engineering makes strides in assistive technologies
Legs, brains, touch and hearing — spotlight examples at #BMES2022
Everyone's everyday sensory, physical, and cognitive experiences in this world are not the same. According to the World Health Organization more than 2 billion people around the world will likely need at least one assistive product by 2030. For individuals with a broad range of disabilities seeking long-term assistance and improved quality of life, promising innovations are on the horizon.
"Technologies and materials are converging to make major advances for rehabilitative and assistive devices," said Grace Hwang, program director for NSF's Disability and Rehabilitation Engineering program.
With the Biomedical Engineering Society's annual meeting this month, here are a few standout examples:
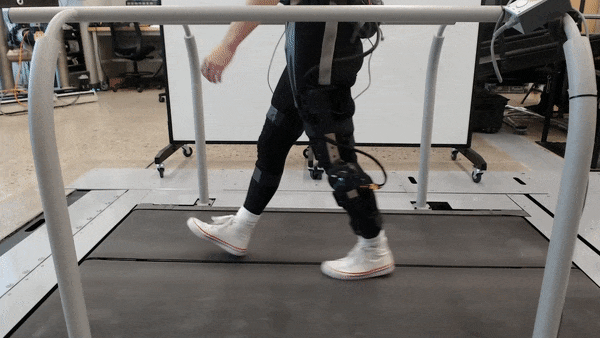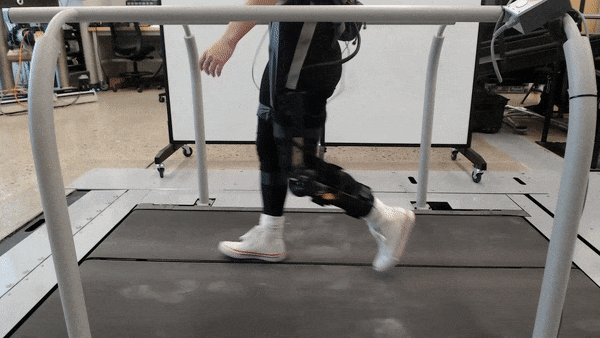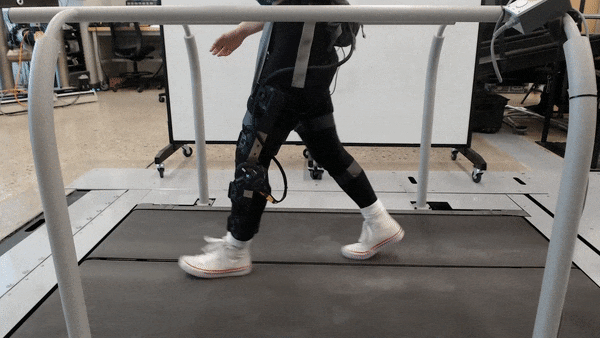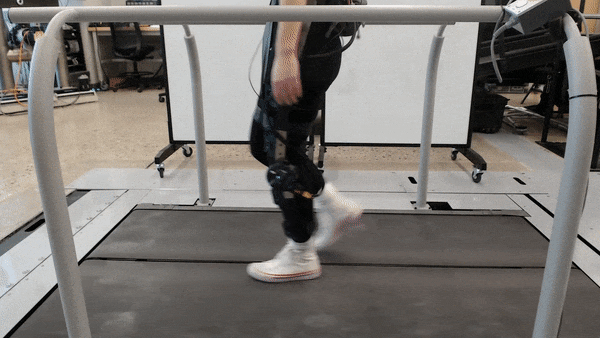
1. Reverse engineering the mechanics of human legs could transform robotic prostheses
Injury at or below the knee can significantly impact movement. Assistive technologies such as robotics and prostheses can help restore mobility lost to injury — even for amputees. But as for adapting to varied, everyday activities, current technologies often underperform.
Researchers in the lab of Elliot Rouse at the University of Michigan have designed a custom exoskeleton to measure the changing properties of the knee, or mechanical impedance, during complex tasks that mirror real-world situations. With NSF support, the lab has accurately estimated the stiffness and inertia of the knee joint during movement. The team hopes to use this knowledge to develop new control strategies for future rehabilitation robotics.
2. New tools convey the complex sensations of touch
The sense of touch is fundamental to the human experience, but little is known about how our perception of touch connects to specific physical stimulus. Current haptic devices meant to mimic touch in virtual reality cannot generate the full range of sensations that we encounter in our daily lives.
With support from NSF, researchers in the labs of Darren Lipomi and V.S. Ramachandran at the University of California San Diego have developed new organic actuators — responsive materials that can recreate sensations of roughness, softness, moisture and adhesion for the wearer. Though made of small polymer structures, these actuators can survive wear and tear for real-world use. New technologies that allow users to naturally "feel" virtual objects could be used to improve simulators for virtual reality-based rehabilitation and for surgery.
3. Soft robot can improve safety and accuracy of placing cochlear implants
The cochlea, a spiral structure in the ear, is critical for hearing. A cochlear implant is an electronic device that rehabilitates hearing difficulties due to damage in the inner ear. However, current electrode implants are limited by stiffness. Rigidity may cause further damage during implantation deep into the cochlea.
Engineers in the labs of Jaeyoun Kim and In-Ho Cho of Iowa State University have devised a new method for safely implanting electrodes in the cochlea. With NSF support, the team developed new robotic actuators that can precisely deliver flexible hearing-aid electrodes into the ear. To avoid harming the cochlea, the actuator is composed entirely of soft materials with embedded touch sensors. Kim and Cho envision that their work will lead to new classes of human-safe soft robots to improve medical interventions for patients.
4. Reanimating paralyzed arms with robotics and electrical stimulation
Individuals with spinal cord injury often need assistance to perform daily activities. This help often comes from functional electrical stimulation, or FES, and assistive robotics. However, FES is not accurate enough to aid fine movements, and assistive robots are too bulky and require too much power. But there's promise in combining the two techniques.
A team led by Marcia O'Malley of Rice University and Eric Schearer of Cleveland State University is unifying FES and robotics to create assistive wearable technologies for upper-limb rehabilitation. With NSF support, the team has developed an experimental technology that combines FES and assistive robotics. This hybrid test bed has demonstrated better efficiency and accuracy than the individual techniques alone. The team's advancement could lead to new, lighter assistive exoskeletons that can help paralyzed individuals perform everyday tasks.
5. Engineered neural networks show promise for restoring brains after stroke
There are no existing methods to fully restore function after a stroke. Stem cell therapies have yet to yield clinical results. Brain-computer interfaces and neuromodulation aim to improve neuronal behavior and function, but these methods either bypass the injury or rely heavily on the damaged brain.
With NSF support, researchers in the labs of An H. Do and Zoran Nenadic at the University of California, Irvine, are creating engineered neural networks: lab-grown tissues trained to recognize and decode brain signals. The team aims for their engineered neural networks to be able to communicate with the brain and eventually replace damaged tissue. This novel approach may one day serve as a therapy to help restore neural function to the cerebral cortex after a stroke.
For more, connect with NSF at the Biomedical Engineering Society Annual Meeting this month.
About the authors
Steven Zehnder is an associate program director and Jonathan Kulwatno is a AAAS Science and Technology Policy Fellow in the Division of Chemical, Bioengineering, Environmental, and Transportation Systems in the U.S. National Science Foundation's Directorate of Engineering.